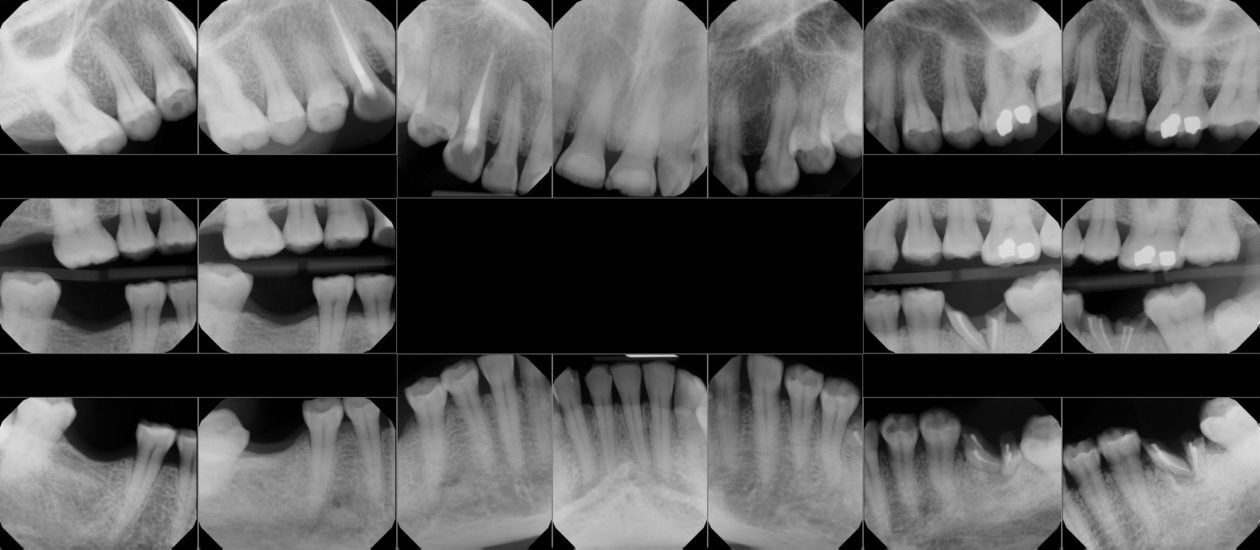
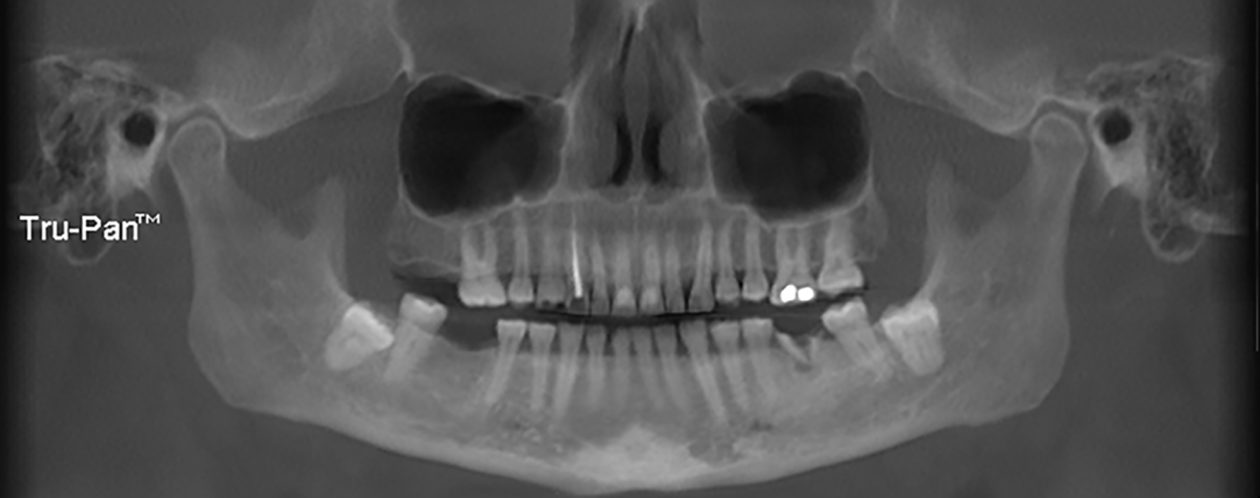
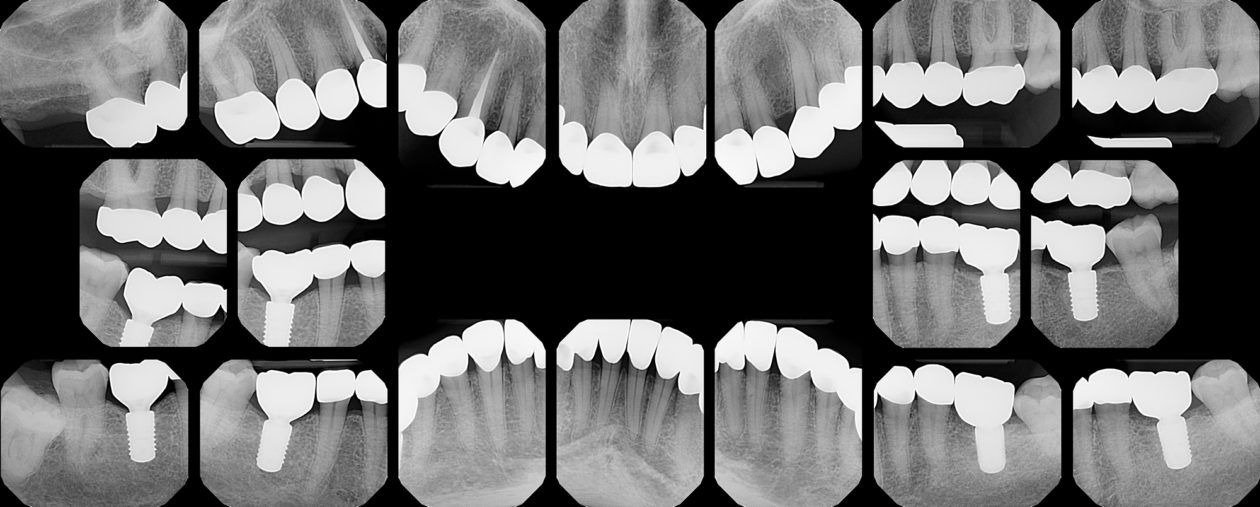
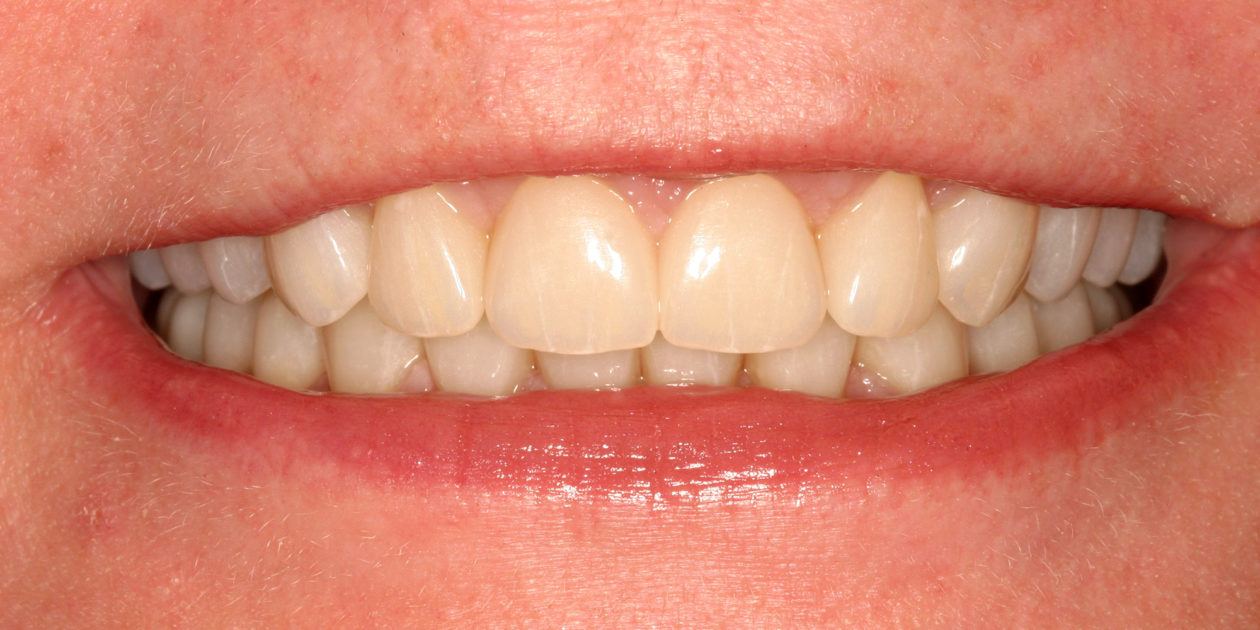
Case 99: Restoration of a Worn Dentition Without Orthodontics
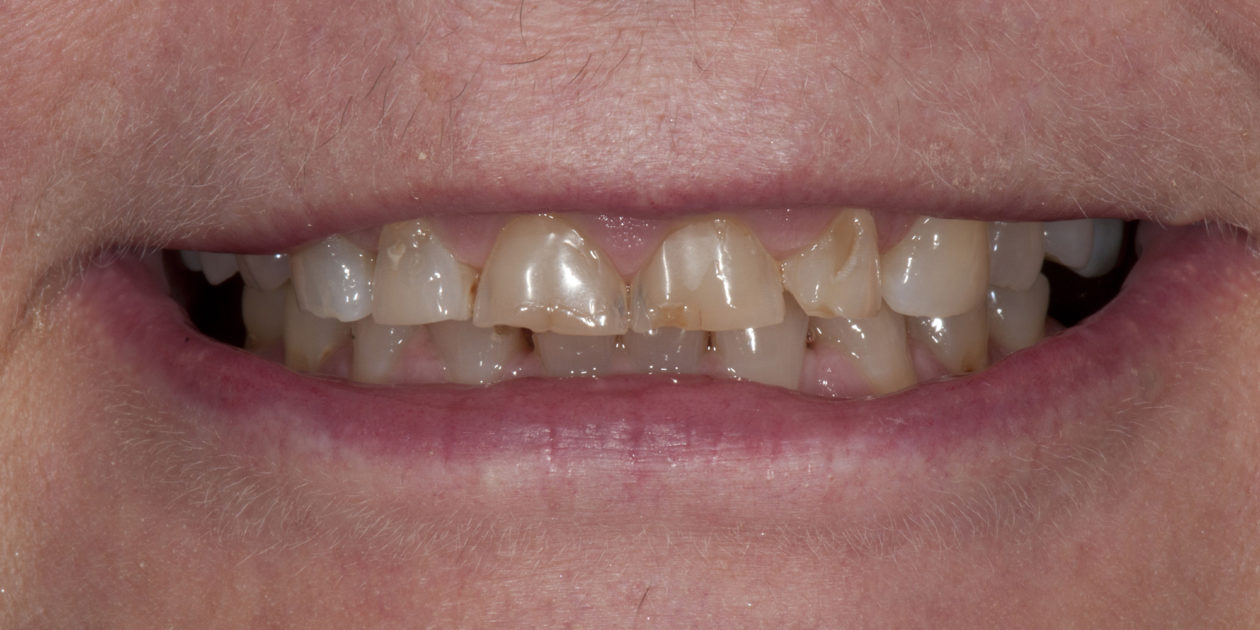
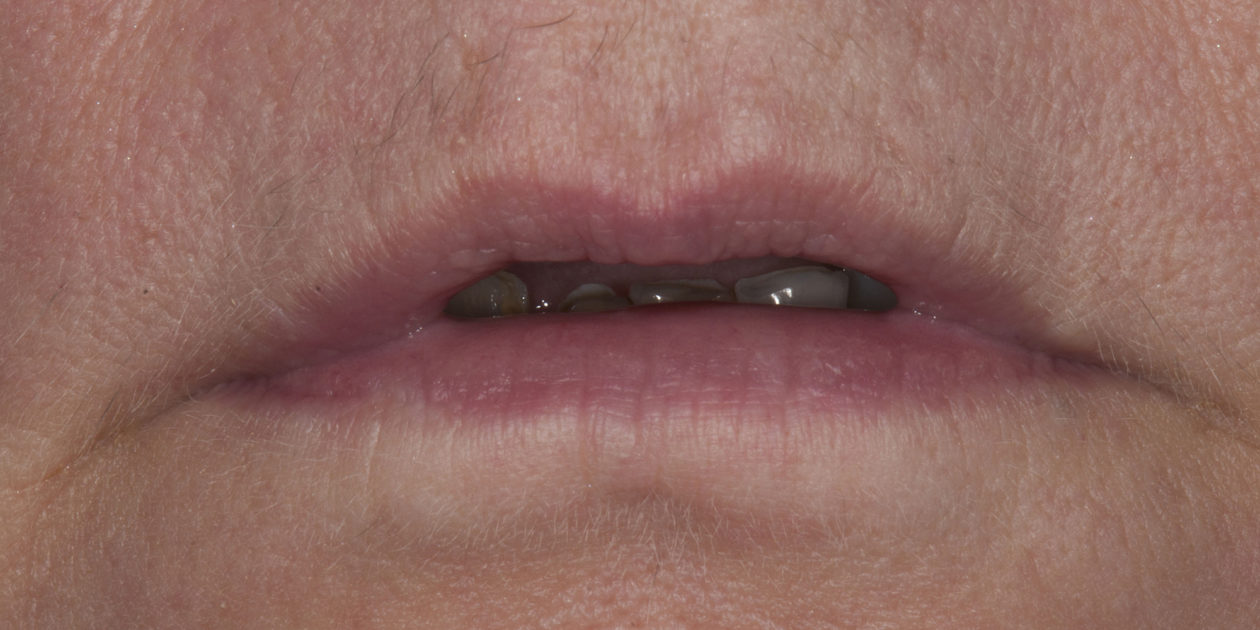
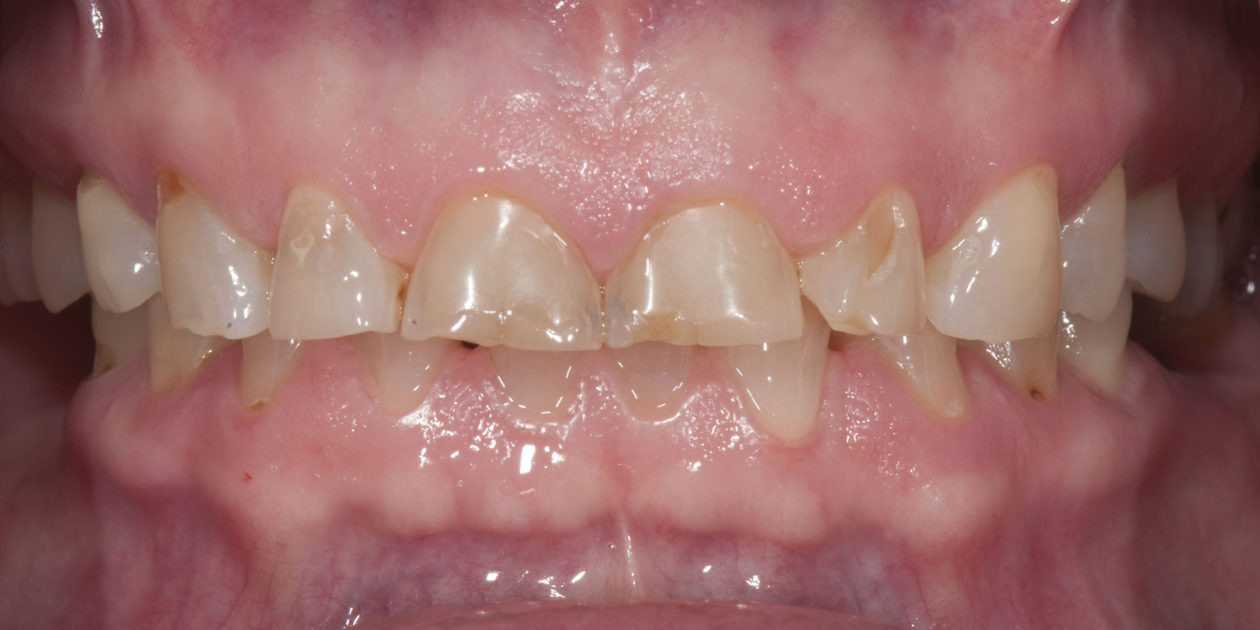
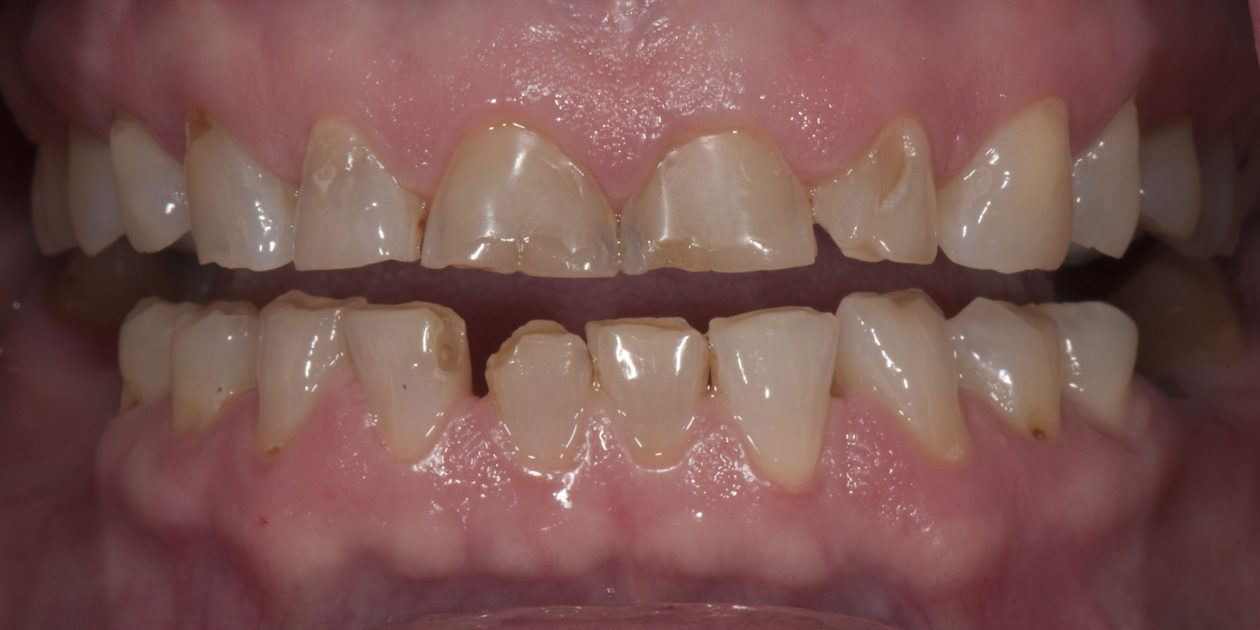
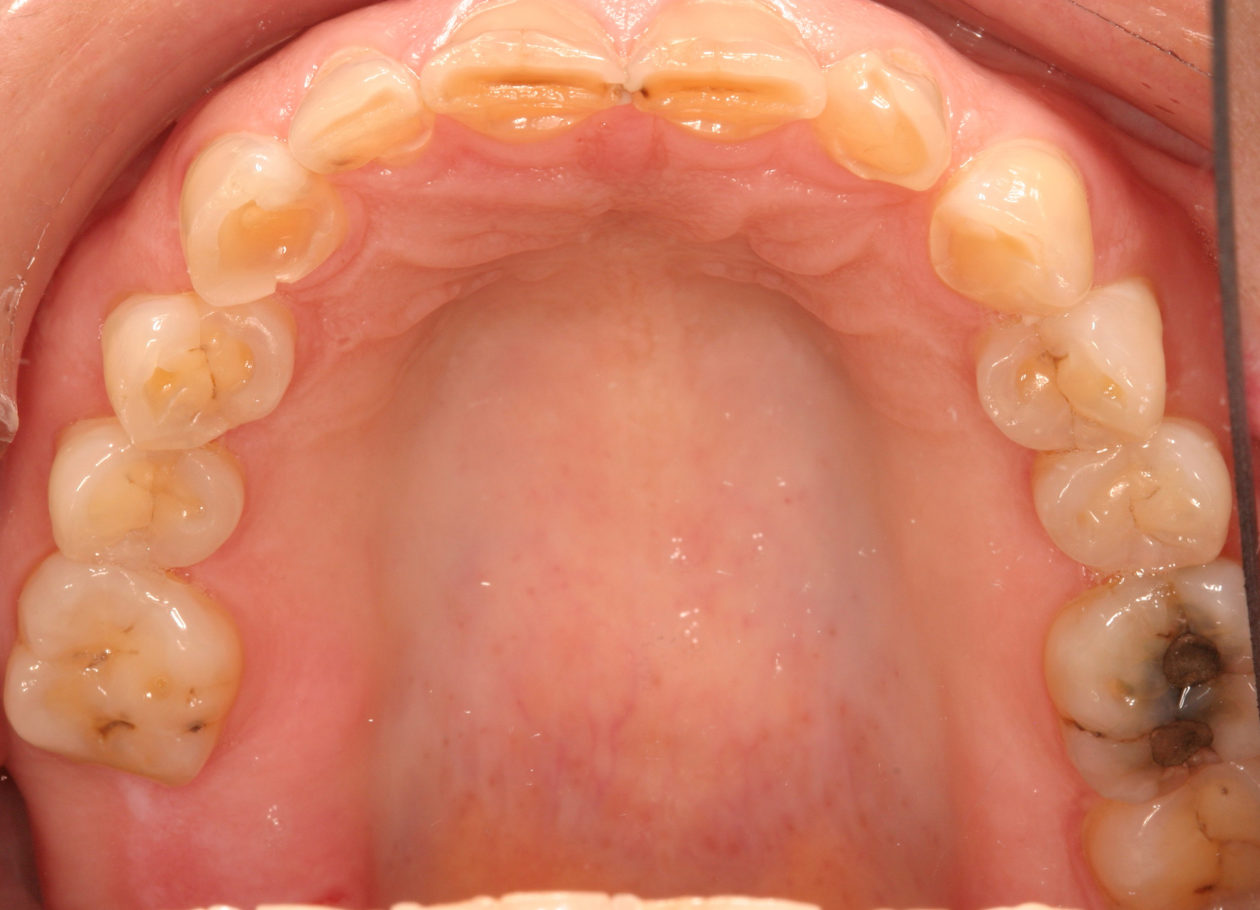
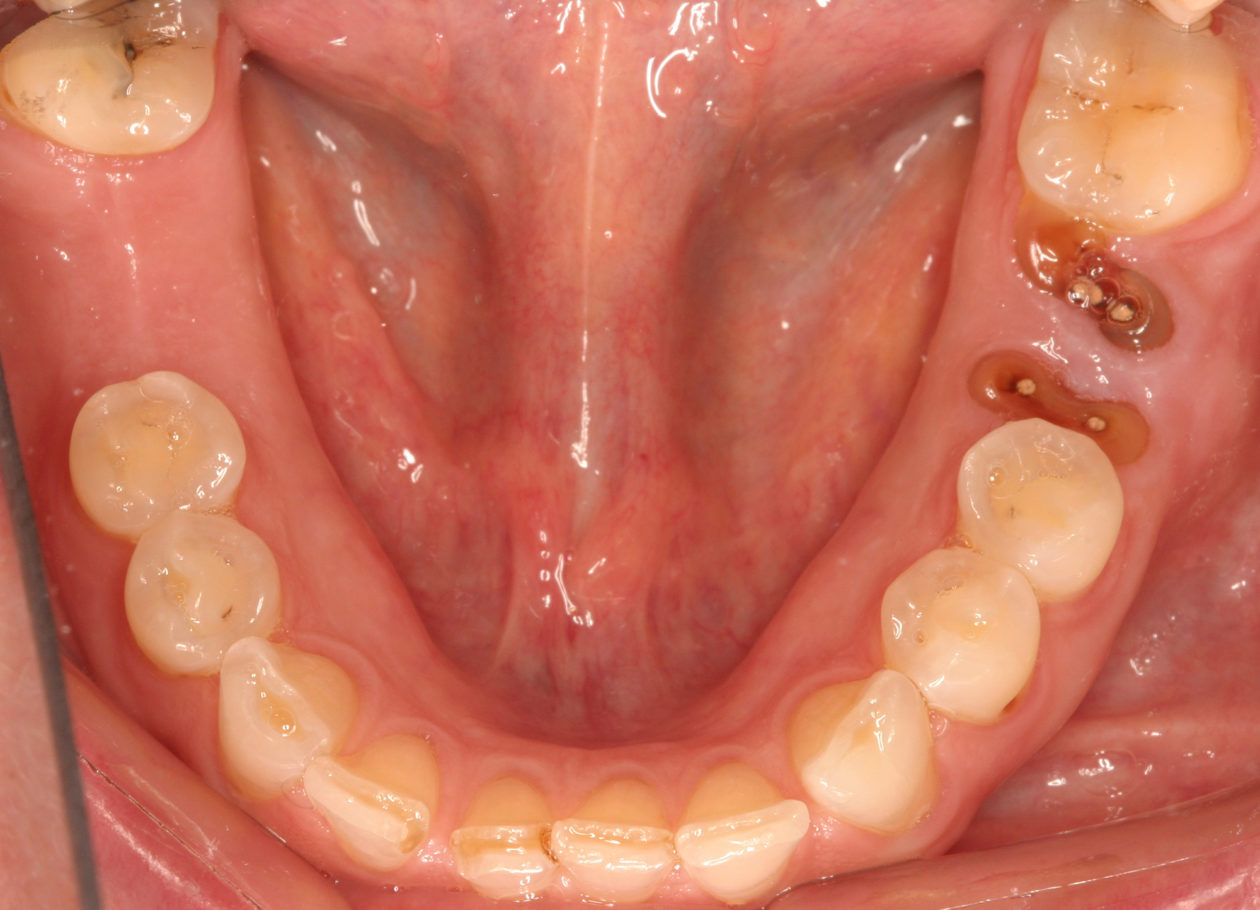
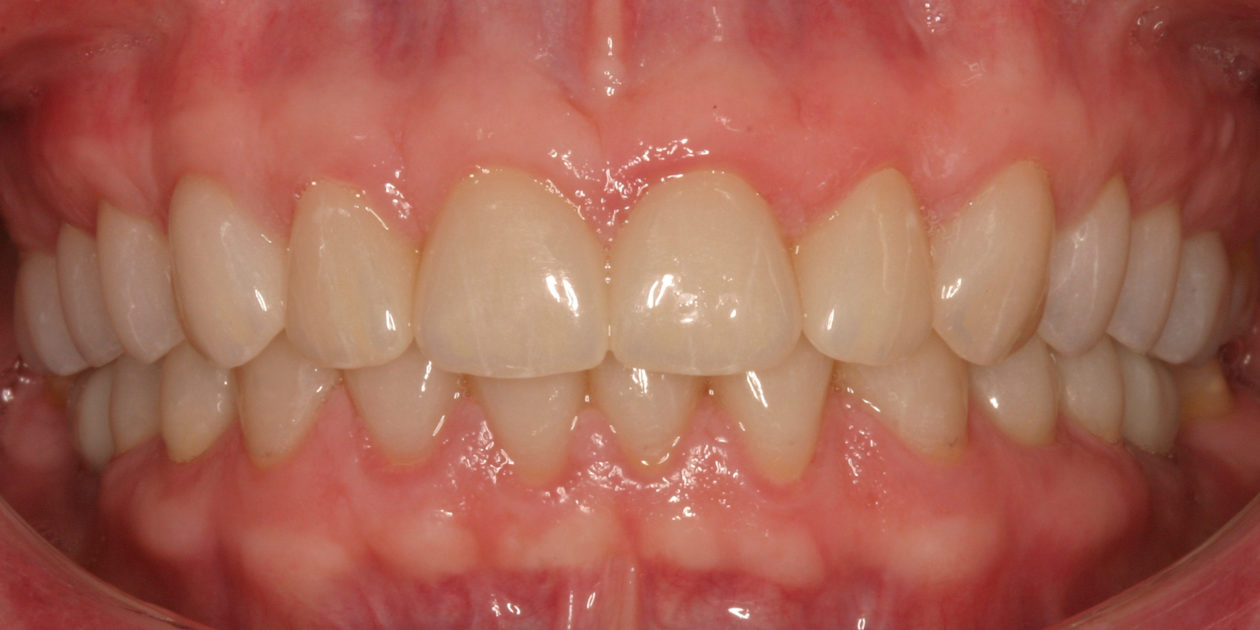
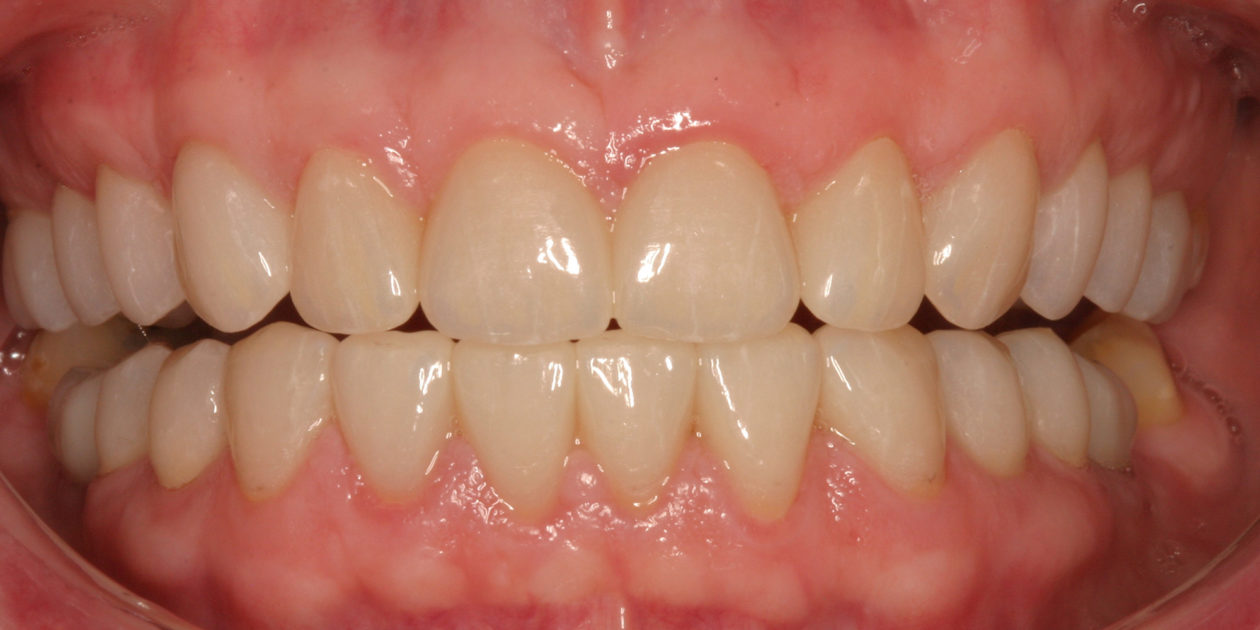
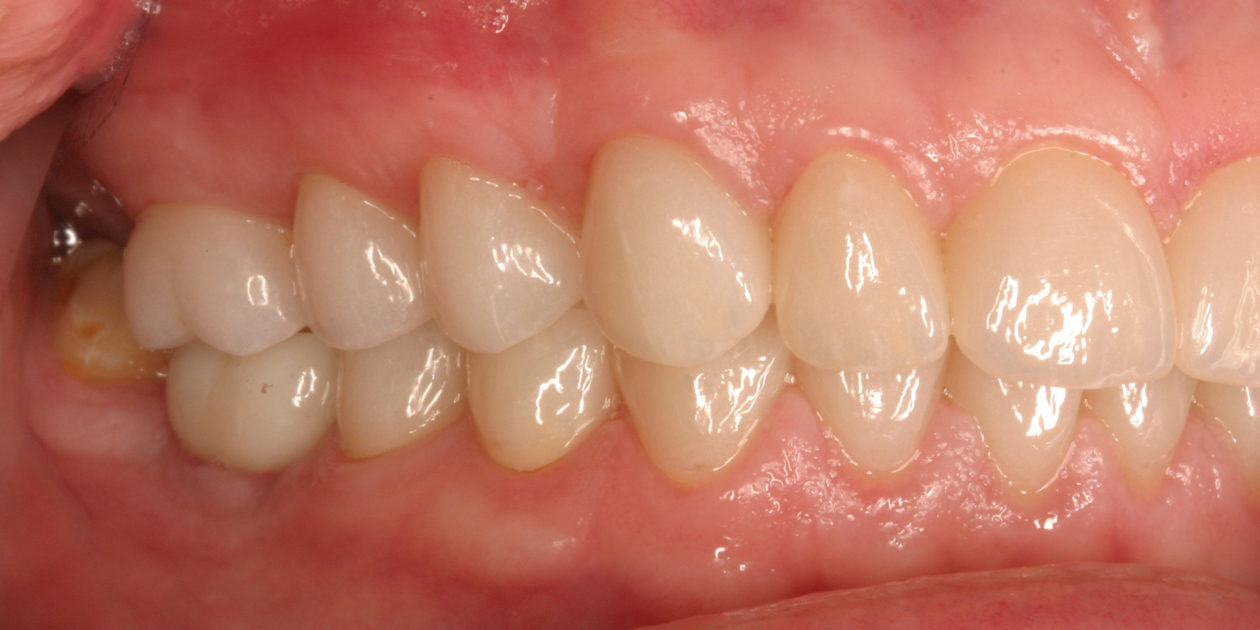
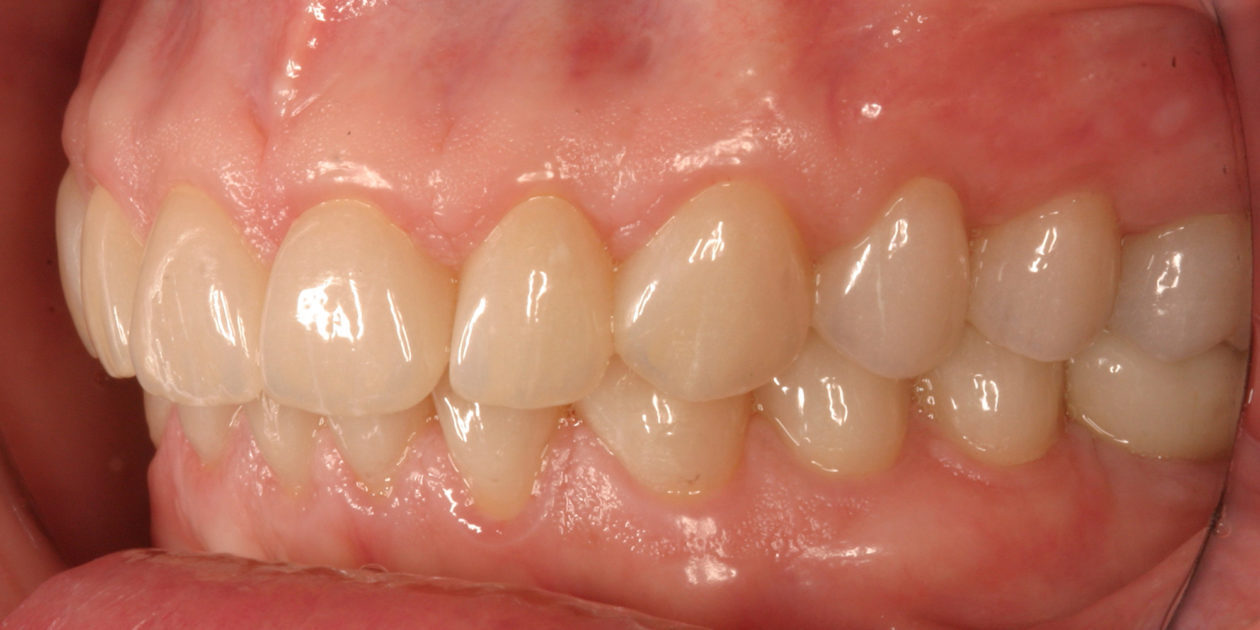
The patient was self-referred to the periodontist’s office. She had not sought dental care for more than 10 years. The patient’s chief concerns included: 1) “My front teeth are chipping and wearing down.”; 2) “I do not want to smile anymore.”; and, 3) intermittent pain associated with tooth no. 6.
After initial treatment at the periodontist’s office, the patient was referred for an endodontic evaluation of tooth no. 6. The endodontic treatment was delayed but ultimately completed nine months later (March 2017). The patient did not return to continue her dental care for an additional seventeen months (August 2018). The patient had become engaged to be married and was highly motivated to proceed with comprehensive care.